Portraits Of B.C.’s Frontline Health Care Workers

By April, a quiet had fallen over Mount Saint Joseph Hospital. Elective surgeries were suspended. The halls weren't humming with visitors. And the cafeteria was closed—except to staff who sparsely occupied it to take their socially distanced breaks. For Robynne Peters, an operating room nurse at the Vancouver community hospital, Mondays, Fridays, and every day in between were bleeding into one another. "I couldn't tell you the date, most days," she says from behind a mask. "It's only on Saturday that you feel kind of normal again."
That was just over a month after the World Health Organization declared COVID-19 a pandemic and British Columbia, along with the rest of Canada, was still expecting the worst. Since then, the province has had success in controlling the outbreak within its borders. It's an accomplishment health-care workers, trained to meet the threat on the front line, continue to fight for.
As with many of her colleagues, the donning and doffing of personal protective equipment punctuate Peter's days. She wears the gear for several hours at a time to shield her from the novel coronavirus, a potentially deadly and terribly infectious pathogen that scientists the world over still struggle to understand.
But the safety measure has a tendency to leave its own mark. "It's like a suction cup on your face," she says while unfastening the mask. "When you take it off, it's kind of embedded in your skin, and you can actually feel it pop off of you."
For others, such as Scott MacKeigan, the workdays leave their mark on the inside, where anxiety can linger long after a shift ends.
He also works at St. Paul's Hospital, a downtown referral site that, like Mount Saint Joseph, is operated by Providence Health Care. There, in the intensive care unit, MacKeigan has seen critically ill patients who have been intubated and ventilated in the battle against the disease.
"Some days you'll go home and think 'I did something right today,'" he says. "That's a good thing. But other days," he adds quietly, choking back tears, "you'll go home and say, 'Something got missed.' That's the hardest part."
Charged with watching over the welfare of their patients, many of the health-care workers at Mount Saint Joseph speak of nursing not as a career, but as a calling.
Tina James has been a cook, a prison guard and a member of the Armed Forces. But for the last three years, she has served as a licensed practical nurse at Mount Saint Joseph Hospital. It's the one career, she says, that she got to choose for herself.
Floating between the hospital's surgical, acute-medicine and COVID units, James says that these days, more than ever, nursing is about more than just medicine. It's the impression she leaves on her patients' lives when close contact with friends and family is generally discouraged.
"It's heart, it's understanding, it's reassurance, it's—oh my gosh—it's washing hair and providing everything," she explains. "You're everything to your patients right now."
But it's also hard, she says. At the end of the day, many of the nurses have families waiting for them at home, some of whom can't afford to be infected. Hanging heavy over their heads is the risk they pose, as potential vectors for the virus, to loved ones.
As a precaution, MacKeigan says, both he and his wife have a basement suite that they've chosen not to rent out while the public health crisis looms large. That's where he will quarantine himself if he ever faces a particularly risky shift. They've both had kidney transplants, he explains, which leaves them immunocompromised and vulnerable to the disease.
Despite taking all the necessary precautions, some at the hospital have still been touched, one way or another, by a virus that doesn't respect pre-existing conditions—or borders.
Peters adds that her mother, in South Africa, was diagnosed with COVID-19 in early April, and died from complications connected to the disease later that month.
Even if they were in the same city, safety protocols likely would have prevented a final visit. Beneath all the protective gear, Peters carries the weight of that loss too. "I'm living with that as well as doing this," she says.
All photographs by Jimmy Jeong
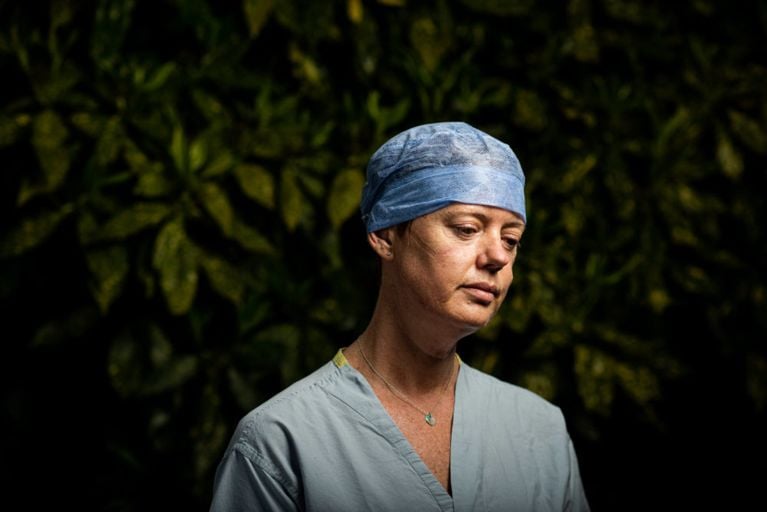
“Everybody is being way more cautious. PPE is being worn all the time. Our surgeries are taking longer because we’re protecting our patients and protecting ourselves, which means we’re doing fewer surgeries during the day.” —Robynne Peters, 46, registered nurse, operating room
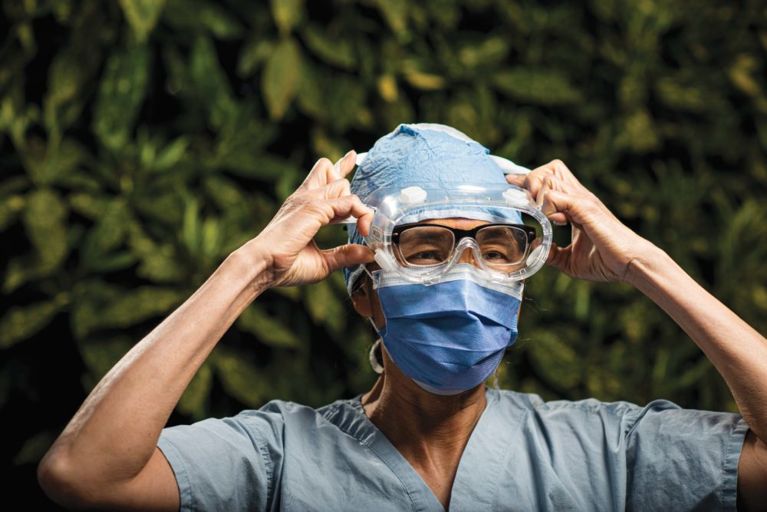
“It worries my family. I also worry about being a silent carrier as a health-care worker, so I’m totally careful. I’m hanging my jacket up outside the house. I shower before I leave work. I shower again when I get home. It sounds OCD, but that’s the way to protect them.” —Sorhwa Teo, 60, clinical nurse leader, emergency department
“We come in with a bright face. We just do what we can and help other people that are in need. This is why we’re in this division, and in a hospital like this.” —Irene Reddy, 51, patient care attendant, geriatric psychiatry

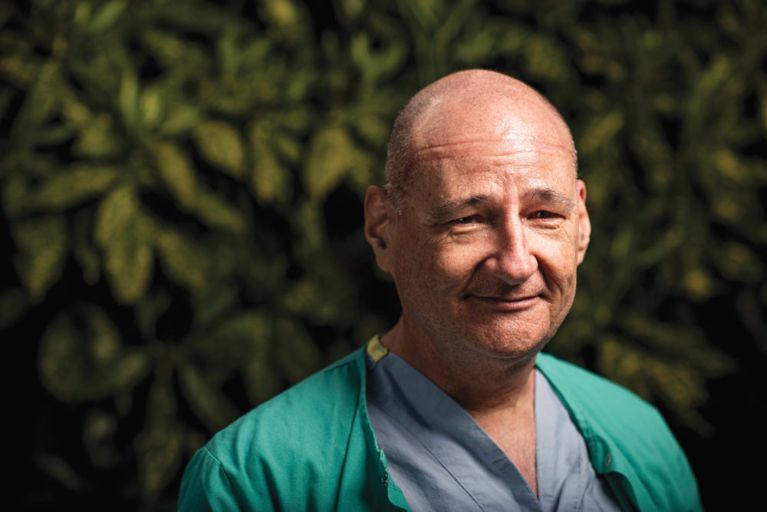
“I appreciate the time that you get to spend with families and the patients. You always want to see somebody get better, but you also go in there with the understanding that they may not. Just being as straight as you can with people is what wins them over more than anything else.” —Scott MacKeigan, 57, registered nurse (emergency department at Mount Saint Joseph; intensive care unit at St. Paul’s Hospital)
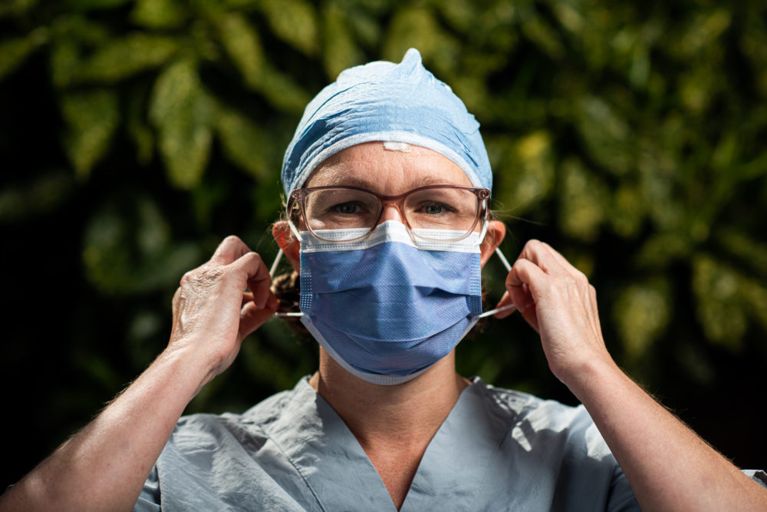
“They (relatives) can’t actually come in and be with the patients, so that support is not there for them. We do whatever we can do, but I feel that is one of the hardest things for patients who really need their family to be with them during this critical time.” —Nasrin Kherani, 64, registered nurse, surgical day care, post anesthetic care unit, endoscopy unit

The hardest part is the unknown, because you don’t know what you’re going to encounter when you step through that door. I have three kids and my husband is also a nurse here, so it’s really high risk.” —Claire Ausa, 46, critical care nurse, post anesthetic care unit, surgical day care

“There might be a few elderly patients that we get that are, of course, needing their family beside them. But because of the pandemic, nobody can come in to stay with those patients. You have to be there at the bedside to help out with what they need.” —Gemma Reyes, 46, registered nurse, medical unit

“We work with a geriatric population, so they are already quite vulnerable. Adding mental illness to the mix makes things like isolation more complicated.” —Judy Wright, 28, registered psychiatric nurse, geriatric psychiatry

Christina Polson, 42, clinical nurse leader, emergency department
“I’m actually self-isolating pretty severely when I’m not here. My husband is a critical-care flight paramedic. We have kids at home from age four to 21, so our family is on full isolation.” —Christina Polson, 42, clinical nurse leader, emergency department
"I can find the resources or where to send these patients that are deteriorating when we don't have the resources as a small hospital. Our resources are limited, so if they need more help, or a specialty or anything like that, I can help facilitate.” —Jojo Agtarap, 45, clinical site coordinator

“When you’re working with COVID-19 patients, and you’ve got people at home that are high-risk, then it’s bound to make you worry a bit more.” —Tina James, 47, licensed practical nurse, surgical unit

Staying at home also plays a big part in keeping everyone safe. Even though you feel like you’re not doing anything, it’s actually a big part of what we’re doing as well. By staying home, you’re actually helping us.” —Reagan Szeto, 28, registered nurse, surgical unit, medical unit

"The hardest bit is seeing the stress of the elderly. There are restrictions, so often their family members can’t accompany them into (the emergency department)." —Fiona A., transition services coordinator, St. Paul’s Hospital and Mount Saint Joseph Hospital

“The only thing I miss is the relationships—the closeness. I hate the distance.” —Mary Luk, 59, registered nurse, post anesthetic care unit, surgical daycare, Mount Saint Joseph Hospital

GET CHATELAINE IN YOUR INBOX!
Subscribe to our newsletters for our very best stories, recipes, style and shopping tips, horoscopes and special offers.